Five signs that you might have Lipedema
Most doctors think you're just fat.
When I look back at old pictures of my mother, especially after she had my older brother at age 21, her thighs and butt looked large and heavy compared to the rest of her. All my life, I figured I had just inherited a “pear shape” from Mom—a ten-inch difference between my stomach and hips.
I had always gazed with jealousy at my petite friends because I had this disproportionately large behind, and very heavy upper thighs that I could never diet and exercise away. My torso was about a size 8, while my bottom was a size 12-14.
But I made peace with it. It could be worse, right? My weight never fluctuated much. I was health-conscious, a runner. I stayed relatively the same through three pregnancies and into middle age. It never became a problem until 2018 when I hit age 50, and my calves, inexplicably, began to swell with fluid at the ankle.
It was a terrifying sight, since I had just watched my father die of congestive heart failure, in which one of the prominent symptoms is edema. I rushed to my doctor, who looked at my legs and said, laughing, “well, it isn’t that! But it’s only going to get worse, and the only treatment is compression.”
She meant compression stockings, and I was devastated. Nothing says “old lady” like compression stockings.
Wearing them 12-16 hours per day is a huge adjustment, and it also means a transformed wardrobe and a transformed lifestyle. No more jeggings or slim-fit jeans—you’re wearing straight leg pants in the winter and long, cool skirts or maxi dresses to hide your hosiery in the summer. You can forget sandals and the beach, unless you like the feel of sand in your pantyhose.
BUT WHAT WAS THE CAUSE? AND WAS THERE A FIX?
At first, I had hoped that the swelling was caused by the thick varicose veins on my legs, and my GP referred me to a private-practice vascular surgeon who treats veins in new ways that are not covered by Medicare here in Canada.
But it wasn’t.
After being treated with a new procedure called Vena-Seal (cyanoacrylate glue is shot into the bad veins to permanently seal them—to the tune of $4,000 per leg), the edema didn’t go away. At a follow-up meeting, the surgeon informed me that he thought the swelling was caused by the fat disorder Lipedema, but my form of the disease was “mild.”
I was devastated.
At the time, my 80-year-old mother had recently been diagnosed in the hospital with Lipedema stage 4. She’d lived her whole life with it and didn’t know it. She had never understood why her bottom half was so large and heavy, why diets didn’t work, why her legs swelled uncontrollably. Over time, her lymphatic system became permanently damaged because the fat in her legs captured so much lymphatic fluid that the skin split open. It couldn’t stretch any more. The lymph fluid (which is part of the circulatory system and is composed of white blood cells, fat and other materials) had been seeping straight through the skin and falling to a puddle on the floor. This had led to a dangerous infection that required hospitalization, and her resulting diagnosis, using lymphoscintigraphy.
I didn’t want to admit that the vascular surgeon was right—that I had Lipedema, too—but instinctively I knew it was true, however mild. And all bets were off for the future.
Researchers estimate that though 11 percent of women worldwide have Lipedema at varying stages (according to Dr. Karen Herbst at the University of Arizona, this means one in nine women in the U.S. alone), it is unrecognized by the average North American doctor, who usually doesn’t differentiate it from obesity.
TREATMENT, PROGNOSIS and COSTS
There isn’t any cure, because Lipedema involves interrelated systems that aren’t yet well understood. Researchers believe Lipedema is likely hereditary and genetic. It involves metabolic processes, the lymphatic and venous systems, and disordered fat production in the limbs. They are looking for better ways to diagnose the disorder.
The only treatments for the resulting edema in the legs are a special form of decongestive massage, which is performed by only two massage therapists in my city (at $90 per hour). Decongestive therapy is rarely covered by private insurance. And in the hospital system, massage therapy is offered by one or two therapists (to mostly Lymphedema patients), plagued by a long waiting list.
The other important conservative treatment is the aforementioned continual wear of medical compression stockings. If you are small enough to wear a standard size, they will run you around $180 each, and must be replaced every six months. Because my mother is much larger and her disease is far advanced, hers must be custom made, and cost $1500 each, lasting 18 months. Medicare coverage varies from province to province--you get three or four pairs a year in British Columbia, for example, but none in New Brunswick. Amounts covered on private plans also vary.
Thirdly, though diet and exercise won’t get rid of the fat, an anti-inflammatory diet and gentle regular exercise are very important to maintain mobility as the disease progresses.
WHAT ABOUT SURGERY?
Twenty years of data gathered by doctors in Germany seems to show that a special form of liposuction is very useful in reducing pain, slowing the progression of the disease, and reducing the volume of fat. Contrary to prior thought, preliminary studies are showing that when the fat is removed, it doesn’t grow back. This form of liposuction is performed by only one plastic surgeon in Toronto for early-stage women, but the surgery can cost upwards of $15,000 and is not covered by Medicare.
But provincial health care agencies believe that liposuction is only a cosmetic procedure, and that there is no proof that it is an effective treatment for the debilitating effects of Lipedema.
Women are forced to pay out of pocket for a procedure that is not covered by private insurance—if they have the cash, or access to credit. It’s no small thing to borrow $15,000 plus expenses (or upwards of $20,000, if you go to the US or Germany for treatment).
But I’m going to do it.
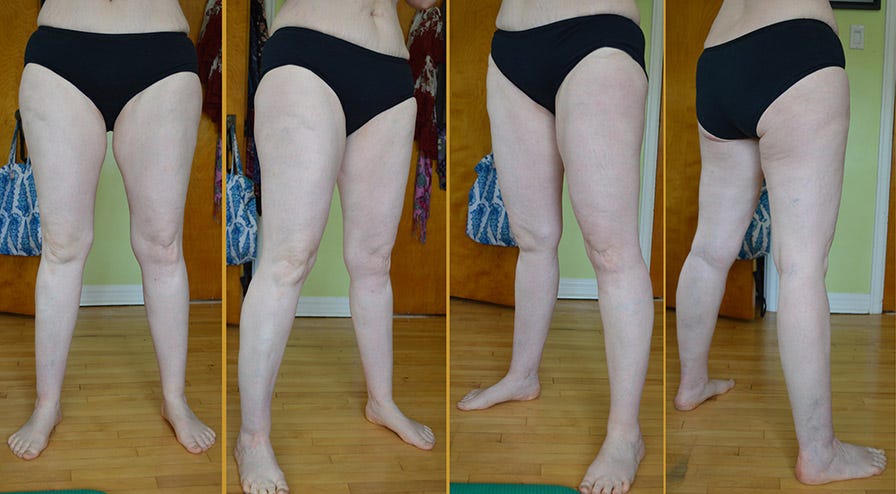
My surgery is scheduled for May 5, 2020. I don’t do this lightly—I’m not looking forward to it. I've thought about the nine-page consent form for a year, and I’ve weighed the pros and cons. But thinking back to how my mother’s condition progressed exponentially after menopause, I want to take every option available. I've already gained ten pounds since these photos were taken a year ago, with no changes to my diet or exercise.
I'll keep you posted on the results.
Five signs that you might have Lipedema
1. Symmetrical subcutaneous fat growth in the legs, stopping at the ankle (and in 30 percent of cases, on the arms, stopping at the wrist). The fat can feel grainy, like rice, or lumpy like walnuts under the skin, and is impervious to diet and exercise. It usually appears at puberty, taking a leap in development during childbearing years, and then again at menopause.
2. The fat is painful to the touch. For some people, the pain is everywhere and for some it only hurts when pressure is placed in certain spots. As the disease progresses through four stages, the legs stiffen and ache after too much walking or sitting in one position.
3. Hyper-flexibility: I remember being in Brownies when I was very young, and we were doing a unit on fitness. I was more flexible than almost anyone. I could put my feet over my head and touch the floor with my toes while lying down, legs straight (I can still do this, at 52). Laughing, the leader said, “I think we can bend her in almost any direction!” Back then, I thought this was something to brag about. I can bend my elbow behind my back and reach the upper middle to scratch, for example, or touch my head on my knees with my whole hands touching the floor, and I can easily push my hands past my feet while seated on the floor.
4. Easy bruising in the extremities. Since I was a kid, I noticed that I would bruise easily on the legs, and the bruises always lasted for a long time. It didn't take a very hard knock to leave a mark.
5. Symmetrical edema in the legs. (Different from primary lymphedema, which is a disorder which usually only involves one side of the body.) There’s likely nothing wrong with your heart. In fact, you might have the blood pressure of a teenager, even if you have a BMI of more than 35. In early stages, the edema builds during the day and goes away after a night’s sleep, but in later stages the lymphatic system is permanently damaged. By stage four, the disease is considered lipo-lymphedema.